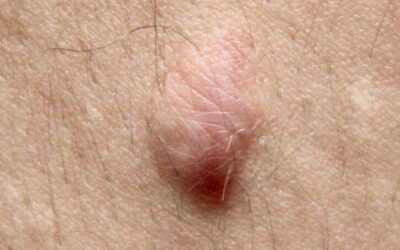
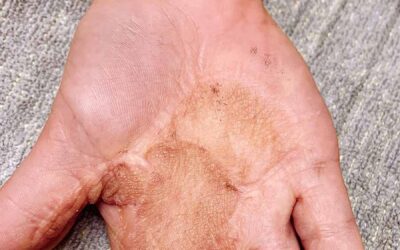
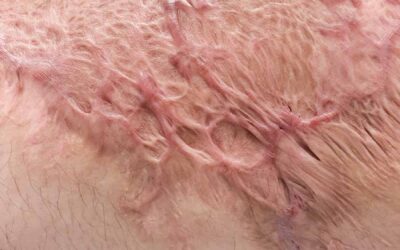
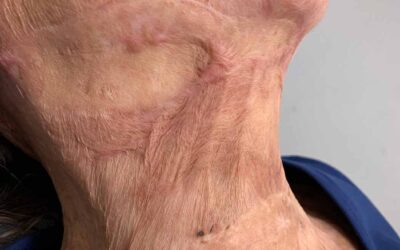
Scar hypertrophy is caused by an overproduction of collagen during pathological (non-normal) wound healing. Scar tissue usually becomes thicker than the surrounding healthy skin during the first months, this normally reduces over time. Increased scar thickness is often called hypertrophy. Burn scars frequently remain hypertrophic to some extent, but scar atrophy (the scar being lower than the surrounding skin) also can happen in some scar.
Category: Scar Characteristic
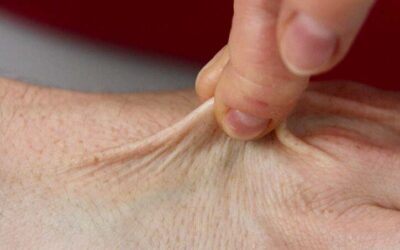
Pliability
Cutaneous scars are required to glide and stretch with healthy skin for normal physiologic function, especially near joints. However, scars are generally stiffer than normal skin. This is mainly because the scar is thicker and has an inferior collagen quality. Pliability is a term used to represent the reduced extensibility of the collagen fiber network and the amount of mechanical tension in the scar. This stiffness may cause limited joint mobility, pain and a sensation of ‘stuckness’ or ‘stiffness’ in the tissues.
Pain
Scar tissue pain is a common condition which can be acute or chronic. Scar pain is caused by damage to small skin nerves, or entrapment of a nerve in scar tissue. Scar pain after surgery can be due to a neuroma (an overgrowth of nerve tissue). Scar pain can be particularly common after operations to repair hernia’s or following surgery to the breast, lung, heart, kidney, and shoulder. Patients with scar tissue pain typically complain of neuropathic (nerve)pain, this may involve continuous pain alternating with sudden stabbing pains in the scar area. Some scar pain may start a number of months post-operatively, after a symptom free period. Scars can also suffer from altered sensation and can feel numb, have strange sensations (such as the sensation of spiders crawling) or be hypersensitive (pain/discomfort when the scar is touched in ways that would not normally be noticed, such as when touched by clothing).
More common than nerve involvement is pain from the scar directly: inflamed, tight, dry and stuck scars can hurt especially if stretched.
Medications may be prescribed for neuropathic pain and/or scar pain, please discuss the options with your doctor.
Itch
As skin heals from a burn injury, it may get itchy. Most people recovering from major burns have problems with itching—especially on or around the burn, graft, or donor site (area where the skin graft was taken from). The medical term for itchiness is “pruritus” (proo-ri´tus).
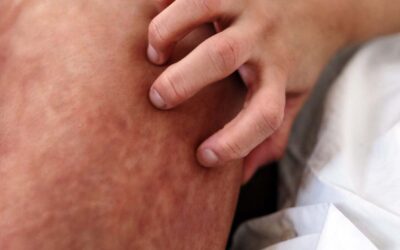
Redness
Redness is seen almost immediately after any form of wounding, whether due to surgery, trauma or a burn. Typically, redness is due to the inflammatory response and the vasodilatation of blood vessels and an increase in their permeability. Most scars become less red at or approximately 7 months after wounding. However, significant numbers of scars, particularly as a result of excisional wounds, remain red still at 12 months. Persisting scar redness isn’t due to ongoing inflammation or infection but may be related to a combination of the overall number of blood vessels within the scar, speed and intensity of blood flow and the level of oxygenated haemoglobin. Scar redness is an important characteristic to assess because it shows how well the scar is evolving or maturing; it often also determines the type and dose of treatment.
Pigmentation
Although local blood supply and pigments such as bile and carotene can contribute to skin tone, the main contribution to human skin colour is melanin. This pigmented biopolymer is produced by melanocytes and distributed in the upper layers of the skin and acts as a physical barrier to protect the skin from harmful solar ultraviolet radiation. Pigmentation disorders in scars are a result of abnormal wound healing and depend on the width and depth of the wound. Abnormal pigmentation can make scars much more noticeable. Scars can be hyperpigmented (darker) or hypopigmented (lighter) than your non-scarred skin. Hyperpigmentation is due to a short inflammatory phase early in the wound healing phase of large/deep skin defects by increasing deposits of melanin to regain balance in the skin. Hypopigmentation results from chronic or extended inflammation, oxidative stressors, and exogenous bacterial or viral presence leading to melanocytes (the cells that produce melanin) not able to make pigment. Re-pigmentation of scars also depends on the presence of hair follicles.
Texture
Scars can form an uneven texture when the dermis (deep, thick layer of the skin) is damaged. The body forms new collagen fibres to mend the damage, resulting in a scar. The new scar tissue will have a different texture and quality than the surrounding tissue, due to excessive production of collagen. An injury with damage to various skin depths which heals by secondary intention also causes abnormal collagen synthesis; this leads to a variety of thicker and thinner bundles. Eventually this results in an irregular scar surface often seen in large surface burn injuries. Irregularities of the scar surface (surface roughness or texture) are also seen after split skin autografting, especially if the skin graft is meshed (holes are made in the skin graft). With a meshed graft, the irregularities result from secondary healing of the interstices (holes) of the meshed skin graft. To improve scar texture, especially in older scars, semi-invasive or invasive treatments are required. Treatments like micro-needling and laser therapy often have very effective results.
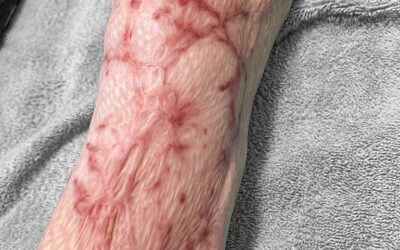
Contractures
Scar contracture is a process that occurs due to an increased and prolonged wound healing response. During the final stage of wound healing (matrix remodelling), the persistent activation of myofibroblasts is a big contributing factor to the formation of scar contracture. Scar contractures will typically appear as fixed, rigid scarring that is confined to the area of trauma. The skin will feel tight and constricted, which can lead to pain, permanent physical disabilities and functional limitations. Deep burns (which lead to greater scarring), especially when over or near a joint can cause contractures. Contractures can be quite common after burn injury. Prevention of scar contractures involves surgery (skin grafting) and wound management to speed wound healing times, and therefore reduce scarring. In combination with this lots of active movement, maybe splinting and other advice given by a physiotherapist is important to prevent and treat contractures. Surgical technique is also important: incisions that are placed parallel to relaxed skin tension lines or that may have irregular angles are more likely to heal satisfactory without functional or cosmetic problems.
Burn contractures may be visible by around 4 weeks post burn, but they can continue to improve or worsen over many months post injury and require longer term care to monitor, prevent or minimise them.