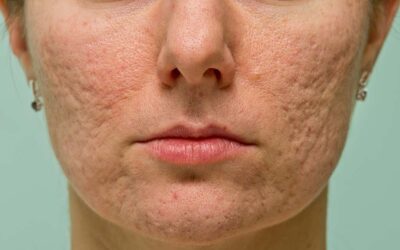
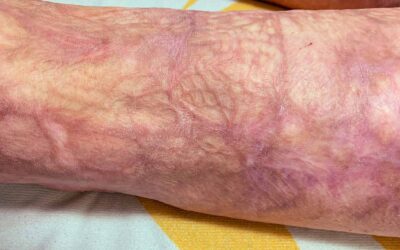
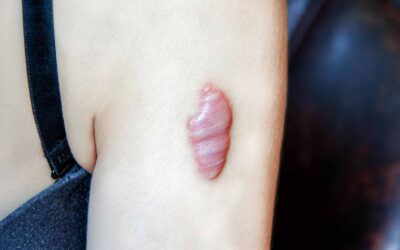
An atrophic scar looks sunken and has a pitted appearance. These scars happen because underlying structures supporting the skin, such as fat or muscle, are lost. This type of scarring is often seen in acne, chickenpox, other diseases (especially Staphylococcus infection), surgery, certain insect and spider bites, or accidents. Atrophic scars can also be common in genetic connective tissue disorders, such as Ehlers-Danlos syndrome.
Category: Scar Type
Linear Scar
Linear scars can be divided in two groups:
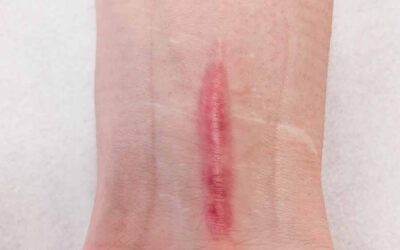
i) Hypertrophic linear scars which are red, raised and sometimes itchy; they are confined to the borders of the original injury. These scars develop within weeks of surgery and may worsen for three to six months before improving. These scars when mature (the process of scar maturation/healing is complete) may be raised, slightly rope-like in appearance and wide. Full maturation can take up to two years.
ii) Stretched linear scars appear when the fine lines of a surgical scar become stretched and widened. These scars are typically flat, pale, soft, symptomless scars and are common after knee or shoulder surgery. Scars that healed with some wound infection or have had stitches that dehisced (burst open) also may be wide, but these scars tend to become hypertrophic. Stretch marks after pregnancy are variants of stretched scars. Unlike hypertrophic scars they are not raised or thickened, and they tend to be smooth rather than bumpy.
Small Keloid
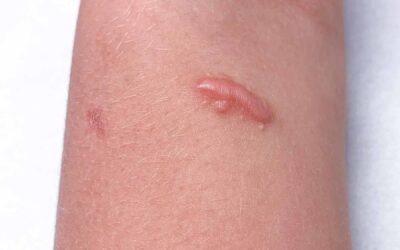
A small keloid is a focused raised, often itchy scar that extends over the normal surrounding skin. It may develop years after the injury and doesn’t improve without treatment. Surgical excision is often followed by recurrence (re-appearance of the keloid), particularly if surgery is not done with other treatments such as radiotherapy.
Hypertrophic Scar
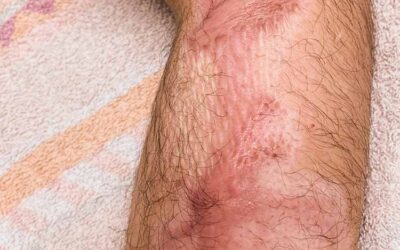
A hypertrophic scar is a cutaneous condition characterized by deposits of excessive amounts of collagen which usually results in a raised, rigid, and red scar. Hypertrophic scars generally develop after thermal or traumatic injury which have damaged the deep layers of the dermis, they are particularly common in areas of high tension.
All scars go through a process of scar maturation, which can take up to 2 years, during this time scars can worsen (get redder, thicker and more painful) before improving. Hypertrophic scars do improve through the scar maturation process, but treatment is often needed to reduce the symptoms during this time and improve the final outcomes.
Burn Scar
Burn scars are usually inevitable when the dermis is damaged and without surgery the wound takes up to three weeks or longer to heal. Although split skin grafts reduce healing times and scarring, they still leave a scar. Even with excellent treatment a scar may be present once the wound has healed. Although scarring can be minimized or improved by various non-invasive, semi-invasive treatments and surgical procedures the scar can’t completely be eliminated. Burn scars are often characterized by hypertrophy, contraction and an uneven texture.
Horizontal Keloid
Horizontal keloids are an irregular superficial spread of hypertrophic and depressed areas. These scars often have a mix of hyper- and hypopigmentation; usually a hypopigmented (lighter) central zone with hyperpigmented (darker) edges. The shape of the scar can be irregular or contractile (e.g., called ‘crab claw’ due to its appearance). A characteristic of these scars is central quiescence (where the centre of the scar appears flattened or mature). All types of keloid scar differ from hypertrophic scars because they can form outside the area of injury, they can be more raised and bumpy than hypertrophic scars.
Vertical Keloid
Vertical keloids tend to be prominent in a vertical direction and look bulbous. These scars usually have distinct borders and a defined shape. There may be limited areas of central quiescence (the centre of the scar is flatter). These keloids may be painful or pruritic (itchy) and can continue to spread over many years.